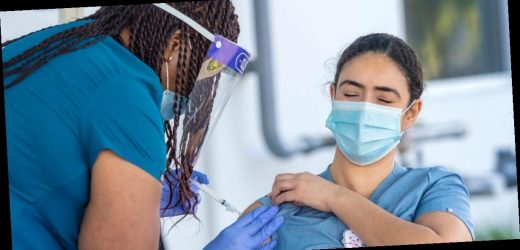
- Two new studies suggest that people who had COVID-19 mount a stronger immune response to their first shot than those who were never infected.
- Other preliminary studies found that people who already had the coronavirus respond to their first shot the way other people do to their second.
- So it’s possible some people might need only one shot to sufficiently protect them.
- Visit Business Insider’s homepage for more stories.
Both Pfizer’s and Moderna’s coronavirus vaccines require two shots: a prime dose, followed by a booster.
The initial shot should trigger the production of antibodies to the virus for the first time. By the time we get a booster, our bodies should mount an even stronger immune response. That explains why some people have reported more side effects after their second shot.
But for people who’ve already had COVID-19, the process seems to progress differently. An emerging body of research suggests that people who already got a coronavirus infection mount a stronger immune response to their first shot than those who never had the disease. That could mean that people with a history of infection don’t need a second shot to sufficiently protect them from getting sick again.
A new study from UK researchers found that antibody levels were roughly the same among uninfected people who received the first dose of Pfizer’s vaccine and people who’d had COVID-19 but weren’t vaccinated yet. Then after people who’d COVID-19 got their first shot, their antibody levels were 140-fold higher than their peak antibody levels before the vaccine.
In other words, the prime dose acted more like a booster.
Another new study found that people who previously had COVID-19 mounted a stronger T-cell response to one shot of Pfizer’s vaccine than vaccinated people who’d never gotten sick did. Like antibodies, T cells have powers of recollection that can help the immune system recognize and re-attack the coronavirus.
But the two studies examined only a small group of vaccinated healthcare workers — 123 in total. For this reason, many scientists are wary of prescribing anything other than the standard two-dose regimens.
“I’m a big proponent of the right dosing and right schedule, because that’s how the studies were performed,” Maria Elena Bottazzi, an immunologist at Baylor College of Medicine, told The New York Times.
People who had COVID-19 may develop 10 times as many antibodies after a single dose
Even before the two new studies came out, preliminary research had started to show that two shots might not be necessary for people who’d already had COVID-19.
In one study, which is still awaiting peer review, researchers at the Icahn School of Medicine at Mount Sinai discovered that people who’d had COVID-19 developed at least 10 times as many antibodies after their first dose as the average uninfected person who received two doses of the Pfizer or Moderna vaccines.
Those with a history of infection also developed stronger side effects after their first injection — including fatigue, headache, chills, fever, and muscle and joint pain.
The researchers wrote that “changing the policy to give these individuals only one dose of vaccine” could “spare them from unnecessary pain and free up many urgently needed vaccine doses.”
Another preliminary study supports those findings — it showed that healthcare workers who’d had COVID-19 had higher antibody levels after their first vaccine dose than vaccinated healthcare workers who had never been infected.
“It was a very large difference. It was something that we could easily see,” Dr. Mohammad Sajadi, an associate professor at the Institute of Human Virology at the University of Maryland School of Medicine, told Insider.
Typically, Sajadi said, COVID-19 patients develop antibodies about two to three weeks after their initial infection. But it didn’t take nearly as long for the people who’d already been sick to develop antibodies in response to a vaccine: These people showed high antibody levels a week after their first shot, peaking about 10 to 14 days after vaccination.
How long does a ‘memory response’ to COVID-19 last?
Pfizer’s and Moderna’s trials suggested both vaccines are safe for people with a history of coronavirus infection. But there are some exceptions.
The Centers for Disease Control and Prevention recommends that people with an active infection wait until their symptoms have resolved and the standard 10-day isolation period has passed before getting vaccinated. That includes people who’ve already received their first dose.
“The recommendations for receiving any dose of the vaccine are not to get it if you’re frankly ill at the time,” Dr. Sandra Sulsky, an epidemiologist and principal at Ramboll, a global health-sciences consulting firm, previously told Insider.
But scientists still aren’t sure when vaccines are actually necessary for previously infected people. Coronavirus antibodies could last anywhere from several months to several years — but even then, antibody levels don’t always translate to immunity.
All the participants in Sajadi’s study, for instance, tested positive for coronavirus antibodies in July and August. By the time they got their shot, he said, some of them had “very, very low levels” of antibodies, but they still seemed to respond strongly to the vaccine.
“What that shows you is that individuals who had a prior COVID infection have what we call a recall response or a memory response,” Sajadi said. “For most infections, the second time you see that microorganism, you should get a faster response.”
He cautioned, however, that the findings apply only to people with a “run-of-the-mill COVID infection” — people who developed antibodies and have recovered from their illness.
An interim solution to limited doses
Sajadi said that giving just one dose to people who’ve already had COVID-19 could help address vaccine shortages. So far, just 47 million Americans vaccinated, with the majority of adults still waiting.
“In times of vaccine shortage, where every vaccine dose counts, we think the data shows if you had previous COVID infection, you may only need one dose for the booster,” Sajadi said. That “may even be the ideal scenario” for previously infected people, he added.
The CDC has said vaccination sites can delay administering a second dose for up to six weeks — instead of the recommended three to four weeks — in “exceptional circumstances.”
It is not yet known how antibody levels among people who’ve had COVID-19 will change in response to to Johnson & Johnson’s shot. That vaccine expected to get authorized for emergency use in the US within days.
“There’s no reason to think it would act differently,” Sajadi said. “But you just never know until you test.”
This story has been updated with new information. It was originally published on February 2, 2021.
Get the latest coronavirus business & economic impact analysis from Business Insider Intelligence on how COVID-19 is affecting industries.
Source: Read Full Article