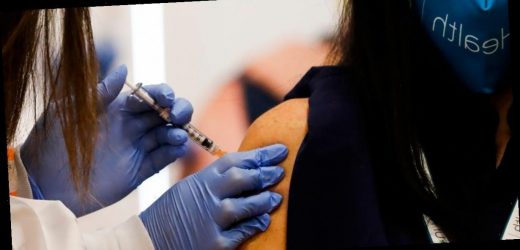
- Pregnant people who are eligible for the coronavirus vaccine have to decide whether the benefits of the shot outweigh the unknown risks.
- There's little data on how the vaccine behaves in pregnant people, since they weren't included in clinical trials, but there's good reason to believe the risks are low.
- Transmission rates, occupation, lifestyle, and risk of serious complications from COVID-19 should all play into your decision to get vaccinated or not.
- Visit Business Insider's homepage for more stories.
Monica Ramirez didn't touch her daughter, Emiliana, until the infant was six weeks old. Emiliana had been delivered via emergency C-section while Ramirez, who had a near-fatal case of COVID-19, was in a medically induced coma.
"I feel very blessed that I have made it," Ramirez, a school staffer near Los Angeles, previously told Insider. "Not everyone has the same outcome."
Had a vaccine been available and given to Ramirez when she was pregnant, her experience might have looked a lot different.
But pregnant people still have a complicated choice to make now that two vaccines are authorized for emergency use in the US.
If they're in a prioritized group for access, like healthcare workers and nursing home staffers, they need to decide: Get the vaccine despite knowing little about its potential risks to them, or skip it and risk contracting COVID-19, which is more likely to lead to complications and death in pregnant people.
Professional and governmental organizations have so far avoided taking a strong stance in either direction, though experts say the way the vaccine is made suggests it's safe in that population.
Read more: Pregnant women aren't prioritized for coronavirus vaccinations, despite being a high-risk group for complications
Ashley McFarland, a 34-year-old registered nurse in Boise, Idaho, says she doesn't know how to help other women make the decision — one she, as a healthcare worker who's trying to get pregnant, will soon have to make herself.
"Even as an educated medical professional, I don't know how the vaccine effects pregnant women and their fetuses," she told Insider. "Hopefully this critical and pertinent information becomes more understood as more research is completed."
Many organizations encourage women and their providers to make individual decisions
The Pfizer and Moderna vaccines, now authorized for emergency use in the US, weren't tested on pregnant people because researchers first want to know how vaccines behave in healthy, non-pregnant people. Only then can they make recommendations about whether certain vaccines should be trialed among expectant parents.
That's typical of any new vaccine, though some experts argue it shouldn't be.
In the meantime, it's largely up to pregnant people who are eligible for the vaccines to decide for themselves if they want to get the shot.
The American College of Obstetricians and Gynecologists, for one, says "vaccines should not be withheld from pregnant individuals" in prioritized groups, while the Centers for Disease Control and Prevention concurs, saying eligible pregnant folks "may choose to be vaccinated."
Both say that while discussing the pros and cons with a provider can be helpful, it shouldn't be required.
The World Health Organization comes down hardest against COVID-19 vaccinations in pregnant people, but provides a critical caveat: "WHO recommends not to use [the Pfizer vaccine] in pregnancy," it says in interim guidance, "unless the benefit of vaccinating a pregnant woman outweighs the potential vaccine risks," like in healthcare workers and those with underlying health conditions.
Pros and cons of getting the vaccine if you're pregnant
Getting the vaccine means being almost entirely protected from contracting COVID-19. If infected, pregnant people have a higher risk of intensive-care unit admission, ventilation, life support, and death than patients who aren't pregnant, though the overall risk is still low, a November report from the CDC found. They're also more likely to deliver prematurely.
Pregnant women of color are particularly at risk for contracting the disease and experiencing related complications.
But getting the vaccine also means taking a bit of a gamble. Researchers don't have good data on the risks to pregnant people, though healthcare and public health professionals expect that they're low.
"Based on how the COVID vaccine works, there should be very little risk to a developing baby," Dr. Jessica Madden, a pediatrician and neonatologist who serves as medical director of Aeroflow Breastpumps, told Insider. That's because, like the flu vaccine, the coronavirus vaccines are do not contain live virus.
"The mRNA in the vaccine acts locally, in the muscle cells surrounding the injection site," she said. "It cannot enter into cells' nucleus, thus it has no effect on DNA."Plus, limited data from animal studies haven't revealed any harms during pregnancy.
Read more: No, the coronavirus vaccine won't make you infertile
But the vaccine could possibly lead to a fever as a side effect, which can be problematic to the developing fetus early in pregnancy. However, ACOG says it can be treated with Tylenol, which is safe in pregnancy and doesn't seem to affect how the vaccines work.
Risk of exposure, pregnancy complications and community transmission rates all matter
Anita Kashyup, a clinical pharmacy specialist in Wauwatosa, Wisconsin, who's trying to get pregnant, decided to get vaccinated after weighing the pros and cons.
"For me, the potential benefits (being protected against getting covid and hopefully then preventing passing it on to others) felt more strongly supported than the potential (unknown) risk with pregnancy," she said, adding that the few women who did get pregnant while enrolled in the vaccines' clinical trials reported no complications.
But other healthcare workers have decided against it, Dr. Zaher Merhi, an OB-GYN, reproductive endocrinology and infertility specialist, and the founder of Rejuvenating Fertility Center, told Insider.
The pregnant people he's offered the vaccine to have by and large turned him down. "For them, it's like, 'I've been fine since March or I got COVID and it's fine. Why do I need to take something that to me, right now, I don't know the risks?'"
"But on the other hand," he added, "they're not seeing pregnant women who are dying from the disease, so it's a battle."
ACOG says the decision should be informed by transmission rates in the community, as well as the individual's risk of severe disease from COVID-19. A pregnant person's occupation and pregnancy complications matter too, Madden said.
It makes more sense, for example, for a pregnant bus driver in a city with high coronavirus rates to get the vaccine than someone who works from home in a small town where transmission is low. Likewise, a pregnant person with gestational diabetes would benefit from the vaccine more than one with a low-risk pregnancy.
But in many ways, these scenarios are theoretical, as for now, most people aren't eligible for the vaccine.
"For women who are pregnant now, but not in prioritized groups, by the time the vaccine is available to them, most will no longer be pregnant," Madden said. "There should be a lot more information available about the safety of the vaccine in pregnancy by the time most of them are eligible to receive it."
For those pregnant people who do have the option, Madden said it's important to consult with a doctor or midwife, but not feel forced into a choice.
"You should feel like your decision is respected," she said, "and please know that if you choose not to get the vaccine right now, or in the future, that it is OK."
If you have a story about the coronavirus pandemic you’d like to share, email us at [email protected].
Get the latest coronavirus business & economic impact analysis from Business Insider Intelligence on how COVID-19 is affecting industries.
Source: Read Full Article