By Aisha Dow
‘A big mismatch’: Manager of access and patient flow Sam Strapps in his office at the Royal Melbourne Hospital in Parkville. Credit:Penny Stephens
Behind a nondescript door on the ground floor of the Royal Melbourne Hospital is a small warren of offices belonging to the bed management team.
The manager of access and patient flow, Sam Strapps, is sitting in front of two computer screens. One shows the demand for admissions and one breaks down the potential discharges for each ward that day.
“There’s often a big mismatch there,” Strapps says.
General medicine staff do the morning rounds at Royal Melbourne Hospital. Credit:Penny Stephens
On this particular morning, a Wednesday in March, they are in the red zone, which means the mismatch is significant. The hospital has yet to reach its likely afternoon peak of demand, but there are already 41 patients in the emergency department needing admission.
“That’s effectively the entire emergency department,” Strapps explains.
At 6.30am, a team of bed managers takes over from an after-hours manager to help get these patients moving. But Strapps says the goalposts are always shifting.
Perhaps five stroke patients arrive all at once, but there are just three stroke beds. There could be more than 100 potential discharges pencilled in at the start of the day, but that drops to 60 to 70 once ward rounds are completed and doctors find patients are sicker than expected.
“That means our original plan might not be the best fit. So we need to put all the pieces back together, but in a different way,” Strapps says.
“We might just say alright, is there anything we can do to expedite the discharges? Are they awaiting a scan? Can I call radiology to say we prioritise this, to get the patient out?”
No matter how dire things look in the morning, Strapps says they always find a way to balance the ledger. On the red days there are regular video meetings with senior staff to talk through how they can improve the patient blockages.
But the red days also seem to be on the rise, and staff from across the public hospital, which celebrated its 175th birthday this week, report they are seeing patients who are sicker and staying longer.
The Age interviewed workers from the Parkville facility this month to talk about daily life in a major Melbourne hospital, in the midst of a long-awaited lull in COVID-19 cases.
8am: General medicine wards
About 20 doctors gather in a conference room. X-Rays, blood results and other patient details are displayed on a big screen, as the night shift staff present the details of notable cases.
The first major business of the day is to talk through any dramas from overnight; any deaths, intensive care transfers, code blues or Medical Emergency Team (MET) calls. The Royal Melbourne Hospital usually averages about 10 to 20 MET calls a day, made when a patient’s vital signs deteriorate worryingly.
“A classic [case] would be a person who has had surgery and then they develop pneumonia or an infection and their blood pressure drops,” says Associate Professor Doug Johnson, the hospital’s head of general medicine.
Johnson says code blues – the highest-level medical emergencies – are now reasonably rare because the hospital has lowered the threshold for MET calls, meaning they are seeing people before they become so sick.
The handover meeting finishes at about 8.30am. The teams from the five general medicine units break off and start their morning rounds, which can continue into the early afternoon. The sickest patients are seen first. They may spend up to an hour with someone who has just been admitted whose cause of illness isn’t clear.
General medicine head, Associate Professor Doug Johnson, speaks to patient Nicholas Leray-Meyer during ward rounds.Credit:Penny Stephens
This area of the hospital is responsible for the largest number of beds. The typical patient is an older person with multiple things wrong with them: diabetes; lung problems; heart failure. It also takes people who have both mental and physical illnesses, including those who have overdosed on drugs, or adults with severe eating disorders.
It may not always sound glamorous, but this section of the hospital is the part often reimagined in US television dramas, where young doctors unravel medical mysteries just in time. Indeed, the general wards at the Royal Melbourne Hospital are the training ground for 130 junior physicians, and it’s the place where patients with mystery illnesses come to be diagnosed.
Johnson says there are usually about two or three “diagnostic dilemmas” within each of the units. Perhaps it is someone with prolonged fever or a patient who is wasting away. Solving these cases, he says, is a “rewarding and fabulous part of what we do”.
Before the pandemic, demand on the general medicine wards would usually ease over summer, to around 80 to 100 patients, and then rise over winter, to about 120 to 130 admissions. But in the last 12 to 18 months there has been no dip, and admissions are now hovering at around 120 to 140. Part of that increase in demand has come from COVID patients, but not all of it.
“Lots of people have theories, but certainly the population is getting older, the population has more comorbidities,” says Johnson. And because people had fewer opportunities to see their general practitioner or specialists during the pandemic, Johnson said people are now presenting with more advanced illness.
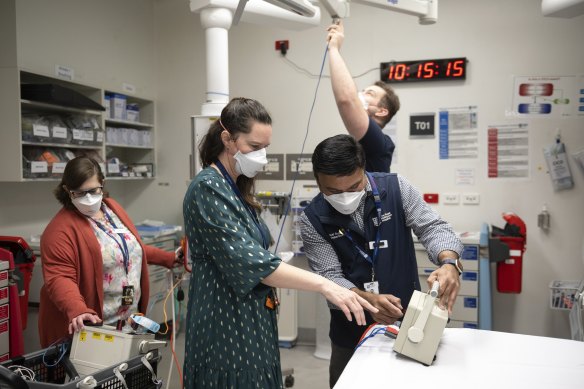
Midday: Central equipment library
Behind a locked grey door, accessible only by swipe card, is a cavernous room. Empty hospital beds are stored in rows and a collection of intravenous drips stand together against one wall. A technician beavers away, making simple repairs and ordering spare parts.
The central equipment library service has been operating at the Royal Melbourne Hospital for about a year. Before that, some wards of the hospital were constantly running out of particular types of equipment, such as bariatric beds for larger patients and infusion pumps that deliver medication and nutrients into the body.
Infusion pumps are attached to patients in the emergency department, and they travel through the hospital with them.
“What we used to see is that emergency would be forever short of pumps, but we would see them stored in other places … And because you could never find infusion pumps, people didn’t want to share them either,” says Dr Rebecca Bailey, the manager of clinical engineering.
“But now we’ve got this central equipment library, there’s just this really great trust that you’re always going to have enough.”
Rebecca Bailey, the manager of clinical engineering, with some of her team in the Royal Melbourne Hospital. Credit:Penny Stephens
The clinical engineering team at the hospital has about 20 staff. Most of the work they do is invisible to patients, but it is vital to keep the hospital functioning. They make sure the medical devices are maintained and manage the buying of new ones within a limited budget.
During the pandemic they began preparing for the worst, auditing the older equipment ready to be thrown out, to see if it could be used a little longer, in the event the hospital and the state was hit by a huge wave of COVID patients. Many of these contingencies were never used, as Australia largely suppressed the virus before vaccines arrived.
However, in September 2021, as Victoria’s major hospitals saw an influx of patients infected with the Delta variant, they quickly created a new 14-bed intensive care pod.
“To introduce a new patient monitoring system … in a hospital is normally a 12-month to two-year process, but what we managed to do was to create a remote ICU that was integrated into that central monitoring system and into the patient electronic medical record in two weeks,” Bailey says.
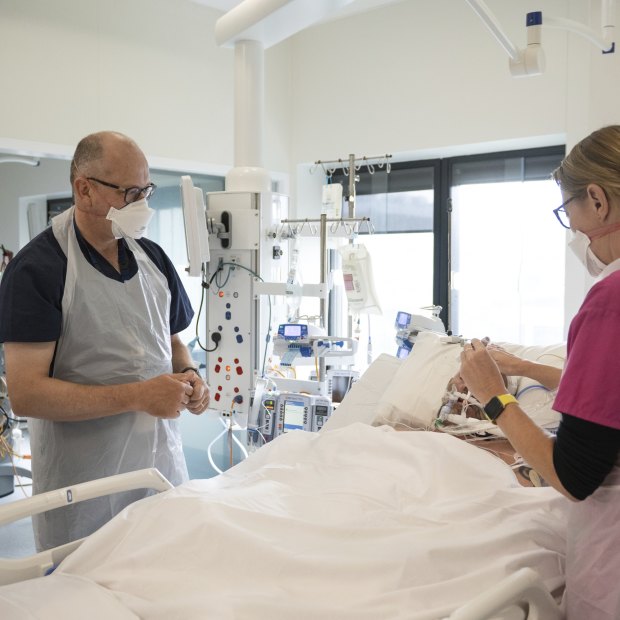
1pm: Intensive care
The intensive care unit at the Royal Melbourne Hospital has only seen a handful of COVID patients in the first weeks of March. Demand from patients with the infectious disease is at its lowest level since July 2021.
But all the 10 extra intensive care beds that were set up during the pandemic are still in use.
“There’s no shortage of work for us,” says Professor Chris MacIsaac, the hospital’s intensive care director. He says the ongoing elevated demand is being driven mainly by increasing numbers of sick patients coming through the emergency department and a welcome return to normal levels of elective surgery.
As a trauma centre, the intensive care unit often cares for patients who have been in car crashes and workplace accidents and men, in particular, who have fallen off ladders.
These people often have significant multi-organ trauma, the most concerning of which, MacIsaac notes, are those with traumatic brain injuries. “They often, unfortunately, have a poor prognosis,” he says.
Because the patients in intensive care are often sedated and essentially unaware of what is happening, intensive care staff put great effort into working with the families of patients, who have found their lives turned upside down.
More than nine out of 10 patients will survive their stay in intensive care.
Intensive care director Chris MacIsaac checks a patient with other staff.Credit:Penny Stephens
For those who don’t, just over half of the families whose deceased loved ones were suitable for organ donation consented last year, resulting in 32 donors from the hospital, whose organs were received by 92 people.
“I think the best thing we can do is encourage people to have that conversation with their loved ones … We all collectively are trying to make the decision that the deceased person would like to have made if they were around, and it’s much easier if they have previously expressed that wish.”
MacIsaac says it is not something he dwells on, but working in an ICU makes you aware that you need to enjoy and be grateful for the times when you’re in good health.
“I think it probably makes you inherently a little bit more cautious,” he says, when asked if what he sees at work changes the way he lives his own life. “You won’t find me on a motorcycle.”
3.30pm: Emergency department
Dr Emma West plops down her bag in the office above the emergency department and takes a quick scan through the list of waiting patients.
The unit is always busy when the evening shift begins. There are sick and injured patients who need moving up to the wards, but there are also more admissions and trauma patients. They have been piling in from about midday.
The question is: Is it standard “super duper” busy or is it “totally out of control”?
“Coming on to an evening shift, you’re arriving understanding it’s going to be busy, you may not get a break at all, and it’s going to require you at your physical and mental best,” West says. “You just don’t have much downtime.”
There has been a sharp increase in the numbers of critically ill people coming into the ED in the past few years. The number of category one cases – those in need of immediate life-saving care – is up 40 per cent since 2019.
If she is lucky, West will knock off at 1am. But if critical patients are waiting to be seen, she will stay on until the situation is busy but “under control”.
The director of emergency medical training sometimes works as the ED’s triage doctor, along with triage nursing staff keeping an eye on incoming patients to ensure they are not losing people with time-critical conditions in the queue, such as those with severe infections that need antibiotics.
Dr Emma West tends to a patient in the emergency department this month.Credit:Penny Stephens
“It’s a mad role,” she says. “You’re pulled in every direction at every moment … You might get three questions a minute and you’re having to process huge amounts of information all the time.”
Part of the job is assessing the patients waiting in the ambulance corridor. Every emergency department in the country has a space like this, even though they are never specifically designed to be used for this purpose. At any one time, day or night, there might be five or 10 patients, or more, laid out on trolleys with paramedics attending.
Among them could be someone in their late 70s who might have a broken bone after a fall. They’re stable but need pain relief and their injuries treated.
Multiple times a shift, the ED doctors will get calls giving them minutes to prepare for the arrival of someone critically injured in an accident – a pedestrian hit by a car or a terrible motorcycle crash. Sometimes they arrive by helicopter. Those patients will get the next cubicle.
“You’re trained over many years to be able to cope with what you see, because it is distressing,” West says.
But amid the distress and the avalanche of cases there are little moments of satisfaction. Word filters through that a young person who had been stabbed in the heart, who they treated five days ago, has been discharged home. Or there is the relief on the face of one patient’s relative when West tells them: “It’s OK, we’re going to look after them.”
The Morning Edition newsletter is our guide to the day’s most important and interesting stories, analysis and insights. Sign up here.
Most Viewed in National
Source: Read Full Article