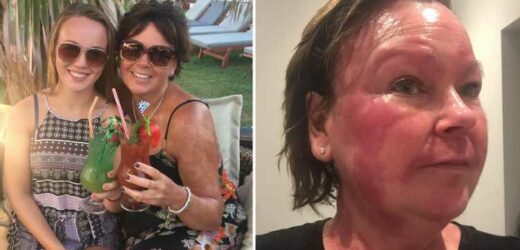
CLENCHING her fists, Lisa Carter winced as her daughter Kaitlyn carefully applied moisturiser to her broken skin.
It had become a painful two-hour routine that she had to carry out multiple times a day.
The 51-year-old, from Crewkerne, Somerset, had been diagnosed with a condition called folliculotropic mycosis fungoides – an extremely rare type of cancer – just days before the UK went into lockdown in March 2020.
It had attacked her skin to the point where her entire body was covered with gaping wounds almost half a finger deep, which needed to be constantly smothered in cream.
Kaitlyn, 20, moved home from university to become her mum’s carer and had only just learned the intensive skincare routine when Lisa sadly died in July last year.
Her body had been unable to fight the constant infections which were able to get into her bloodstream through the open sores and left her too weak to have cancer treatment.
Yet, if detected early enough, mycosis fungoides is a treatable condition with a normal life expectancy.
Now Kaitlyn is bravely sharing her mum’s story in the hope that it will help people get an earlier diagnosis and prevent another family from going through the same traumatic experience.
She said: “The majority of people with mycosis fungoides have a normal life expectancy, so if mum had received an earlier diagnosis her journey would have likely been very different.
“She’d had skin problems for as long as I can remember and consultants had told her it was likely eczema or psoriasis.
“It began as plaques all over her body which were very dry, raised and itchy.
“Initially she managed her condition with topical treatments and ultraviolet light therapy, which seemed to work in the short term before coming back even worse."
Lisa’s condition worsened in the summer of 2019 when her skin started to release large amounts of moisture.
“Although her skin was dry, her clothes and bedding would be soaked within a few hours,” Kaitlyn said.
“She was very good at hiding how uncomfortable she was and continued to look as glamorous as ever, carrying a spare pair of clothes to change into halfway through the day.”
In September 2019, despite her pain and discomfort, Lisa managed to cycle to Paris from London to raise money for the British Skin Foundation.
What is Mycosis fungoides?
Dr Fiona Child, the Consultant Dermatologist who treated Lisa Carter explains…
Mycosis fungoides is a rare type of T-cell lymphoma that involves the skin.
It can occur at any age but is most frequently diagnosed after the age of 50 years.
It often mimics other conditions such as eczema and psoriasis and therefore diagnosis can sometimes be delayed.
It usually presents with dry, scaly patches of skin that may have irregular shapes.
The patches may develop into thicker lesions, known as plaques, and sometimes nodules or tumours may occur, which can break down to form painful ulcers.
In a small number of patients, the skin may become red all over.
Although it is a lymphoma, in the majority of people it is an indolent disease, does not spread beyond the skin and is associated with a normal life span.
However, in a minority of patients it can become more aggressive and ultimately spread beyond the skin.
In those with very widespread disease, where the skin barrier is damaged, there may be an increased risk of significant and life-threatening infections.
The aim of management is to improve symptoms and control the disease as there is currently no cure.
Treatments can clear the rash, but it usually recurs. In the early stages, skin directed therapies are favoured and include topical steroid creams or ointments and phototherapy (ultraviolet light therapy).
Low doses of radiotherapy may also be used for individual lesions and can be used to treat the whole skin surface (total skin electron beam therapy) in those with more widespread disease.
If skin directed therapies fail to control the disease effectively, other treatments may be needed which can range from immunotherapy (drugs which encourage the body’s immune system to fight the lymphoma cells) to chemotherapy.
There are also a number of targeted antibody therapies currently in development or being assessed in clinical trials.
Many research groups from around the world are working together to understand the causes of mycosis fungoides and why it behaves more aggressively in some patients.
The ongoing research will lead to more effective management strategies and improved outcomes for our patients.
But less than two months later her body began to struggle with her temperature regulation and she was forced to give up her beloved job as a school business manager.
Kaitlyn said: “She was constantly freezing, no matter how warm the house was.
“The moisture released from her skin combined with the dampness from the creams meant it was impossible for her to get warm.
“Mum was also beginning to lose her hair and her skin was deteriorating massively, with huge open sores appearing all over her body.
“She knew it wasn’t eczema and her GP had passed it off as menopause. But she pushed to get a second opinion and this doctor actually referred her to see a consultant in London.”
SHOCKING DIAGNOSIS
In March 2020, Lisa went to the St John’s Institute of Dermatology at Guy’s Hospital and finally got her diagnosis – folliculotropic mycosis fungoides.
It’s a rare form of T-cell lymphoma, a blood cancer, which starts in the cells that normally help the body fight germs and attacks the skin.
Kaitlyn said: “None of us expected it to be cancer, but we were slightly relieved because finally we had a diagnosis and she could be treated.”
Due to the severity of her condition, Lisa was booked in to start radiotherapy the next day. But after just a couple of weeks of treatment, she started showing Covid-19 symptoms and was advised to isolate back home in Somerset.
Lisa’s test result came back positive while blood samples also showed she had sepsis from staphylococcus bacteria which had gotten in through her open sores.
She was admitted to Yeovil District Hospital to fight off the infection before she could return to London to continue her radiotherapy treatment.
Kaitlyn and her dad, Danny, temporarily moved to a flat in London so they could look after Lisa – with Danny taking her to hospital in the day while Kaitlyn stayed up at night to do three rounds of cleaning and treating Lisa’s skin.
She said: “Mum was covered in open wounds that were about as deep as a third of my finger and as big as my palm.
“When I was applying the cream I had to wear gloves to be sanitised, but they were too big for me and she was wincing with the weight of that.”
After some improvement, Lisa took a downward turn in May when she contracted another septic infection, which had caused her brain to swell leaving her delirious with slurred speech.
She was taken to intensive care and put on a ventilator, dialysis and into an induced coma.
Incredibly she fought off the infection again and was transferred to a high dependency unit where she spent her birthday.
CONSTANT BATTLE
Kaitlyn says from there it became a vicious cycle of her mum getting better and then being hit with another devastating sepsis infection.
“One minute mum was doing really good and then she’d be in an induced coma with the sepsis,” she said.
“When she was being treated for sepsis, her skin couldn’t be treated and she was too weak for radiotherapy.
“It was a constant battle and put a massive halt on being able to get on top of it because her skin was continuously breaking down.
“But she stayed so positive through it all and she was determined to get home.”
Lisa spent the next few weeks trying to build up her strength and by the end of the month she was able to walk 60 metres, so the plan was to move her back to Somerset.
On July 6, Kaitlyn travelled to London and spent the morning at the hospital in full hazmat gear where she was taught Lisa’s gruelling two-hour skincare routine – which had to be done multiple times a day.
Mum was so weak, she could barely lift her head. When she asked me to ring 999 I knew it was bad because I knew how much she didn’t want to go back to hospital
“I remember thinking, ‘how on earth am I going to be able to do this?’,” she said.
“The amount of bags of cream, dressings and other medication we were sent home with was crazy – it filled the entire boot and backseats of the car.
“One of the most shocking things I had to prepare for her was the burn sheets that lay underneath her.
“They are a sort of mesh underlay to go on the bed that is usually used for burn victims.
“We had to cover them in a cream that felt thick and greasy like lard just to keep her back moisturised.
“That night, me and my nan did her skincare and my two brothers came over and we all just sat with her. It was very emotional but amazing to have her home.”
But in the morning, Lisa took a turn and told Kaitlyn to call an ambulance.
She said: “Mum was so weak, she could barely lift her head. When she asked me to ring 999 I knew it was bad because I knew how much she didn’t want to go back to hospital.
“When the paramedics came they insisted on taking her back to London as Guy’s was the only place equipped to give her the care she needed.”
Sadly, it was the last time Kaitlyn would see her mum.
Lisa had developed yet another septic infection but this time it was too severe for her body to fight and she died in ICU a few days later, with her husband by her side.
Kaitlyn said: “I was ready to go and be there but in retrospect, it would’ve been horrible. It was heartbreaking enough seeing her – she was tiny and had no hair and she didn’t look like my mum.
“The truth is that even if she had beaten this infection, she would have faced another a week later because of how severely broken down her skin was. It was inevitable.
“I feel if she had been diagnosed earlier, her skin could have been treated before it got so bad and things could have been very different.
“But because it’s so rare it can be extremely difficult to get a diagnosis, so I hope that by sharing her story I can stop just one other person from experiencing what she did.”
Source: Read Full Article